The bacterium Legionella pneumophila and related bacteria are common in natural water sources such as rivers, lakes, and reservoirs, but usually in low numbers. Conditions in these environments are rarely favorable for individuals to become infected with the bacteria.
These naturally occurring bacteria may also be found within the built environment i.e. purpose-built water systems. The built environment allows conditions to be maintained within the water system that will encourage growth and transmission of the bacteria, for example:
-
The water temperature may be suitable for bacteria to grow in all or part of the system, this is typically between 20–45°C;
-
It is possible for water droplets to be produced and, if so, they can be dispersed;
-
Water may be stored and/or re-circulated;
-
There may be deposits that can help to support bacterial growth, such as rust, sludge, scale, organic matter and biofilms.
Legionellosis is a collective term for diseases caused by legionella bacteria. The most serious form of Legionellosis is Legionnaires’ disease; which is a potentially fatal form of pneumonia. Legionnaires’ disease is normally contracted by inhaling contaminated water aerosol that is suspended in the air. These very small droplets of water can contain the legionella bacteria.
Although everyone is susceptible to infection, there is an increased risk for the following groups:
-
Increasing age [> 50years. Children are rarely infected];
-
Men [approx. 3x more likely than women, this may change with altered smoking habits];
-
An existing respiratory disease that makes the lungs more vulnerable to infection;
-
Illnesses & underlying health conditions [cancer, diabetes, kidney disease or alcoholism];
-
Smoking [particularly heavy cigarette smoking - probability of impaired lung function];
-
Patients who are immunocompromised as a result of illness or treatment [i.e. those on immunosuppressant drugs that inhibit the body’s natural defences against infection].
Healthcare providers include organisations such as NHS Trusts, Health Boards, and private healthcare companies. The buildings operated by these organisations, namely hospitals, clinics, and surgeries, are often large with complex water systems that can provide the ideal environment for legionella bacteria to proliferate [as detailed above].
People who go to hospital invariably have a complaint that needs medical attention; the visit to hospital can be brief or for an extended period whilst they receive treatment. During their visit, these susceptible individuals could be exposed to aerosols containing legionella bacteria that have multiplied within the building water system. The vulnerable nature of the population results in an increased risk of Legionnaires’ disease.
The Water Safety Group [WSG] needs to introduce sufficient measures & strategies, that do not allow unchecked proliferation of the legionella bacteria in the water systems and reduce, so far as is reasonably practicable, exposure to these aerosols.
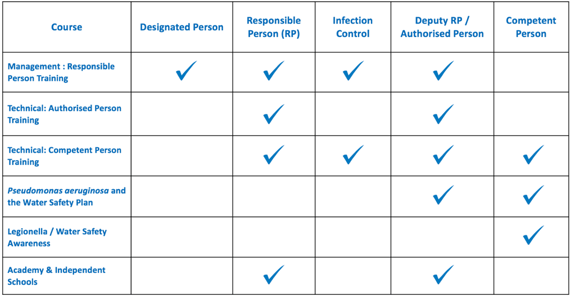
The WSG is a multidisciplinary group of individuals, made up of appropriate experts to ensure all elements of the water safety plan are fully implemented. The individuals can include, estates management, facilities management, infection prevention & control, microbiologist, Authorising Engineer [water], specialist departments, plumbers, contractors to name just a few. The Authorising Engineer [Water] is an independent professional advisor with a defined responsibility for auditing, appraisals, reviews and support.
Read More in our blogs - 'The Hidden Dangers in Hospital Water Systems' and 'Water Hygiene Tips for the Control of Waterborne Pathogens in Healthcare Organisations'